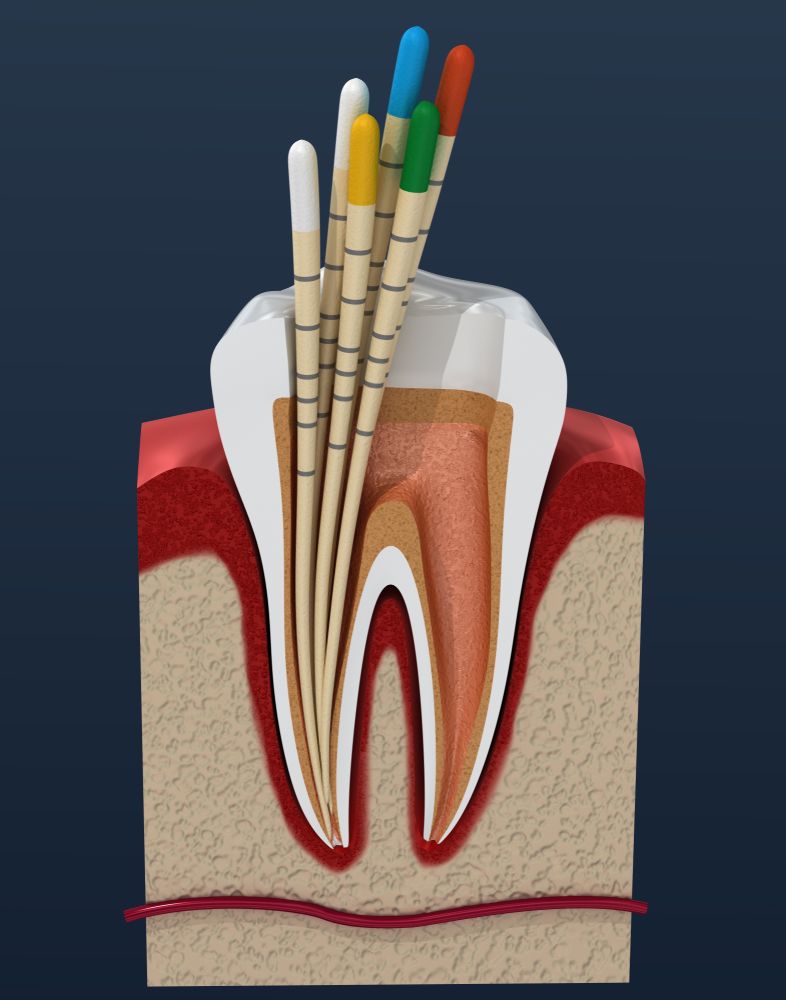
The material used to fill the space after root canals are cleaned and disinfected.
The material used to seal a root canal is gutta-percha. Gutta-percha is a rubber-like compound used for decades to fill root canals and for other medical purposes.
A root canal treatment involves removing the pulp and biological material within the tooth and filling it with gutta-percha. The procedure can be performed on single teeth or multiple teeth. After the gutta-percha has been inserted into the tooth, it’s heated or cooled to harden it, then sealed with a crown or filling.
Filling a root canal begins with numbing agents applied to the area around the tooth to reduce any discomfort that may occur during treatment. The dentist then drills into the tooth and removes any damaged material from inside it before cleaning out all debris inside your mouth, so there aren’t any contaminants left behind when filling occurs afterward! The next step after cleaning out debris is placing a temporary filling into your mouth until a permanent one arrives later on down the road!
Root Canal Sealer Biocompatibility and Cytotoxicity

Several different types of root canal sealers are available in the market. These include Bioceramic-based, methacrylate-based, zinc oxide-based, and calcium hydroxide-based sealers. Depending on your needs, your dentist may use a combination of root canal sealers to prevent future problems.
Bioceramic-based root canal sealers
Bioceramic-based root canal sealer materials are one of the newest technologies in endodontics. These materials are biocompatible and promote bone remineralization by stimulating physiological responses. They also enhance the release of anti-inflammatory cytokines in the PDLSCs.
These materials are available only in endodontic offices. They are considered a beneficial technology in endodontics. Bioceramic refers to materials created specifically for medical use, such as zirconia, alumina, bioactive glass, and calcium phosphate. The bioactive elements in bioceramic materials encourage the growth of tough, durable tissues.
Bioceramic-based root canal sealer materials are known to be effective in preventing reinfection in the root canal space. This is the ultimate goal of root canal treatment. However, the results of clinical trials are not yet conclusive. The lack of randomized clinical trials has led to an inadequate understanding of the effectiveness of bioceramic-based sealers in endodontics.
In vitro studies of root canal sealer materials have examined their physical properties and biological features. They also evaluated their cytotoxicity and biocompatibility.
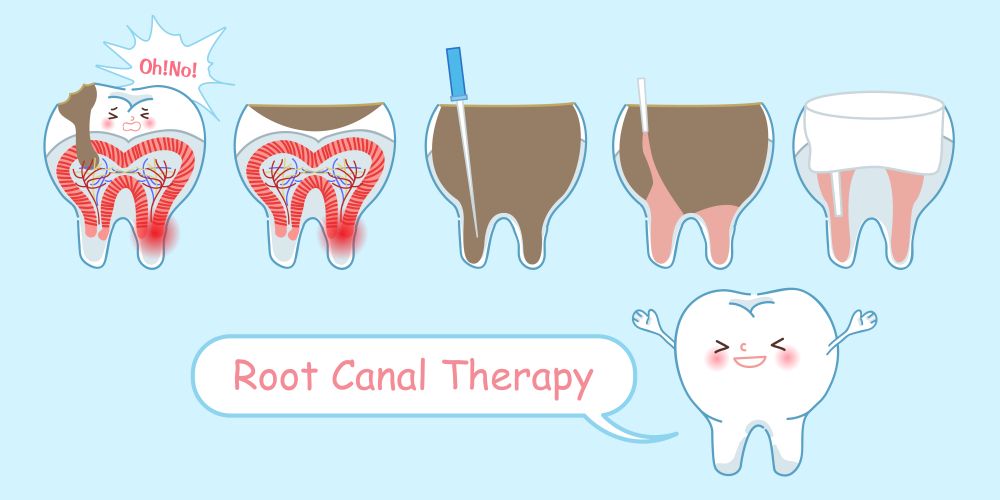
Methacrylate-based root canal sealers
An essential aspect of methacrylate-based root canal sealers is the antibacterial effect. This effect is particularly important because microorganisms such as bacteria are often the culprit of persistent apical periodontitis. Several studies have investigated the antibacterial properties of DMADDM. A current study aimed to develop an antibacterial root canal sealer. Different mass fractions of DMADDM were incorporated into EndoREZ and evaluated for their cytotoxicity and apical sealing ability.
Historically, methacrylate resin-based root canal sealers were not widely used in dentistry. However, during the past five years, methacrylate resin-based root-filling materials were introduced in the market. Due to the increasing demand for bonded root-filling materials, more research has been done on methacrylate-based root canal sealers.
Researchers have studied the solubility of various root canal sealers in chloroform and eucalyptus oil. The sealers were poured into standardized samples and immersed in these solvents for 30 seconds, five minutes, and 20 minutes. The solubility was then determined using multiple paired t-tests.
Zinc-oxide-based root canal sealers
Zinc-oxide-based root canal fillers contain zinc oxide powder and calcium hydroxide or bismuth subcarbonate. They are resorbable, which is suitable for sealing close to vital structures. These sealers also have good antimicrobial activity.
In vitro studies have evaluated the physical and biological features of these sealers. They have also been tested for cytotoxicity. Nevertheless, more studies are needed to establish the sustainability of root canal filling sealers. In vitro testing has also shown that zinc oxide-eugenol-based sealers offer the lowest microleakage.
In one study, researchers evaluated the radiopacity of three zinc oxide-based root canal sealers and one containing eugenol. These root canal sealers showed the highest antimicrobial activity compared to the other two. However, some researchers did not report any significant differences.
The main scope of a root canal sealer is to bind gutta-percha and dentine walls. It is essential that the sealer adheres well to the dentine and gutta-percha. However, glass-ionomer-based root canal sealers had lower adhesive strength.
Calcium hydroxide-based root canal sealers
A comprehensive literature search was conducted to understand the biological and biocompatibility of calcium hydroxide-based root canal sealers. Articles were identified using key terms, including endodontics, cytotoxicity, biocompatibility, and bioceramics. Included articles included studies of root canal sealers that were published in the past five years. The inclusion criteria included original data; exclusion criteria included systematic studies, case reports, and articles with limited data.
The primary purpose of root canal sealers is to fill irregular gaps in the root canal system. Therefore, it is vital for them to exhibit low solubility and disintegration. Dissociation of Ca(OH)2 would compromise its favorable effects on the body. However, calcium hydroxide-based sealers display good sealing ability and are biocompatible with bacteria.
Calcium hydroxide is a biocompatible material that promotes the formation of tooth tissue and the biological sealing of the apical foramen. However, spreading calcium hydroxide within the root canal is difficult due to its insoluble nature in water. Root canals are complex, with several canals per tooth.