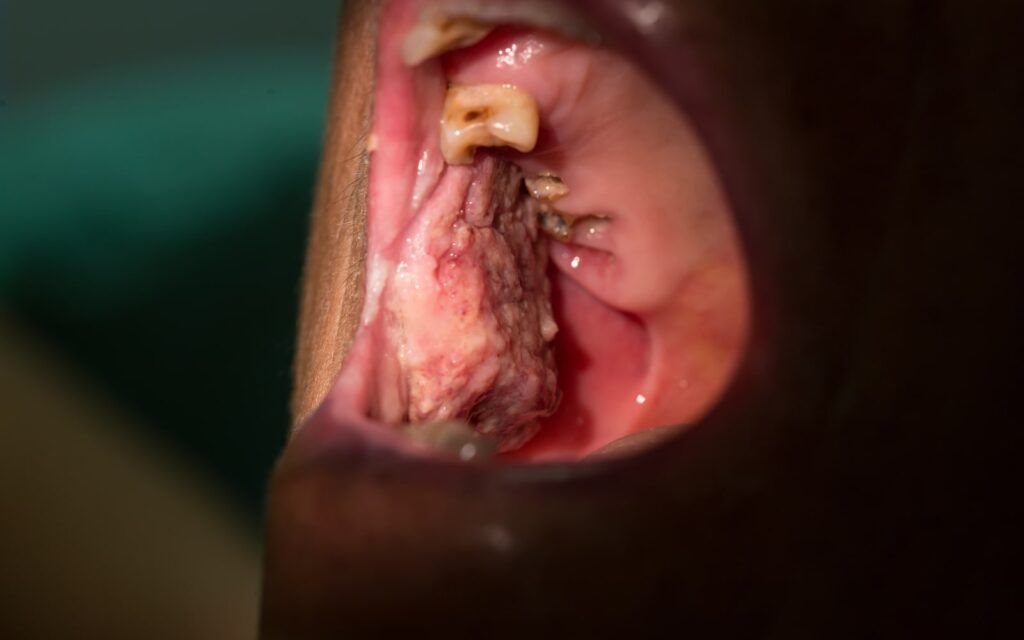
When faced with a potential cancer diagnosis, endodontists have to prepare for this drastic news, especially when the early warning signs appear during treatment. During this time, it is highly important that thorough examinations are performed to determine the type and severity of the tumor and its relation to the oral structures, and even inspect other areas not normally observed for extra precaution and assurance for the patient. Due to their obscurity, oral cancers can occur in many different areas of the mouth and facial regions, which makes diagnosis even more important for both dentist and patient. During these times, endodontists need to have special precautions in place to provide the best resources possible for their patients. To observe this, we’ll be providing a brief explanation of those protocols to help inform patients of the possible outcomes and recommendations when faced with the possibility of oral cancer.
The Types of Oral Cancer and Diagnostics Tools
To provide the best outcomes for dental patients at risk of oral tumors or cancers, dentists in this position need to be able to provide oral cancer tests to locate the affected tissues, observe the state of the tissue, and learn about its behaviors. In cases where abnormal tissues appear during examinations, dentists often use these tests to determine if cancer is present:
- Endoscopy: Endoscopies use thin, flexible tubes to check inside the mouth and throat. The thin tube contains a view lens that allows for more detail to be observed directly to help better locate the tumor, determine its type, and other factors involved.
- Oral brush biopsy: Biopsies allow dentists to submit samples of tissues to laboratories for additional testing. Oral brush biopsies take a small number of tissue cells and are then submitted to a pathologist or oncologist to determine their cellular makeup.
- Barium Swallowing Tests: Barium swallowing tests determine the health of the oropharynx, especially if abnormal tissue growths are present. Through the barium swallowing test, patients swallow small portions of liquid barium to allow the dentist to observe changes within the oral cavity structure. This test also allows dentists to see whether the liquid passes easily to the stomach, observe signs of blockage, and help determine the type of cancer.
- HPV Testing: HPV has been linked to certain types of oral cancer, and thus HPV testing can sometimes be used to determine cancer’s stage, type, and available treatment options.
These tests are often combined with tests such as x-rays, MRI scans, physical examinations, and CAT scans to help dentists observe the different angles, details, and locations of the tumors to determine the cancer type. For dentists attempting to diagnose tumors, it’s important to know what types of cancers could affect the mouth. These cancers include:
- Lymphoma: Lymphoma typically occurs within the lymph node regions and can also appear around the oral cavity.
- Mucosal Melanoma: Mucosal melanoma appears within the mucous membranes found throughout the body, and the mouth is the most common area where this type of cancer is found.
- Sarcoma: Sarcoma cancer commonly affects the tissues such as fat, nerves, bones, blood vessels, and fibrous tissues. Sarcoma cancer can also occur within the mouth but is considered somewhat rare.
- Minor Salivary Gland Cancer: Because there are multiple types of carcinomas, they can also appear within the salivary glands throughout the mouth.
Once the type of cancer is confirmed, the stage and grade of cancer need to be determined in order to determine its severity and growth speed, and from there, treatment options can be brought to clarity. To determine its severity and growth, dentists, alongside pathologists and oncologists, use specific terminologies within a staging system, including:
- “T” for Primary Tumors: This stage, abbreviated as “T” within the system, is used to describe the location and size of the tumor, measured within millimeters and centimeters. Each stage is separated into smaller groups to describe the tumor in detail, including how advanced it is within the area, any nearby structures, invasion into the muscles and bones, and the number of skin and muscular layers the tumor has reached through.
- “N” for Regional Lymph Nodes: The second stage assesses the lymph nodes, marked as “N” within the system. It determines the clinical and pathological infections of the cancer cells within the lymph nodes to determine the speed and rate at which infections can spread according to the body’s immune system response and the potential for fighting off infections during cancer treatments.
- “M” for Metastasis: The “M” stage determines the rate at which cancer spreads. If signs of cancer are seen in other parts of the body, then the cancer is in metastasis.
- “G” for Grades: Referred to as “G” within the system, this stage determines cellular health compared to normal cells. This stage determines the differentiation of the cancer cells and how much they resemble normal tissues.
Managing Oral Cancer Alongside Endodontic Treatment
Patients diagnosed with malignant tumors face numerous challenges, and among those challenges are dental infections. Dental infections are more likely to increase due to the intensity and severity of the treatments involved, and due to existing compromised immune systems, endodontists often have to work with their patient’s healthcare plans to provide the required treatments alongside their cancer treatment to alleviate those symptoms. Because of the increased rate of infections, certain treatments can be applied to help alleviate common dental problems, including:
- Oral Mucositis Management: Oral Mucositis is a side effect of cancer therapy, and the degree of infection depends on the amount of radiation used. Radiation treatment typically results in lesions of the mucous cells, and these lesions can be treated with anesthetics such as lidocaine, benzocaine, dyclonine, and capsaicin.
- Dry Mouth Management: Dry mouth is also a common side effect of cancer treatment, as chemotherapy and radiation therapy often cause irreversible damage to the salivary glands. Early symptoms of dry mouth can be managed with salivary stimulants, cavity treatments, custom administering trays, and diet changes to help assist patients during their cancer treatments.
- ORN Management: ORN, also known as osteoradionecrosis, is exposed bone loss of the mandibular jaw bone, which often occurs during severe amounts of cancer treatment. Depending on the cancer staging, radiation doses and oral hygiene levels, deep periodontal scaling, flap surgery, and other types of restorations are applied in these cases to help restore the mouth back to a healthy state.
To learn more about your available options, visit your dentist, oncologists, and cancer treatment centers regularly for information about types of oral cancers and available dental treatment options.